If you are a Service Member or Veteran with an immediate crisis,
please contact the Veteran Crisis Line at 800-273-8255, text 838255, or
chat with someone at www.veteranscrisisline.net.
These signature wounds include painful symptoms such as flashbacks, avoidance, isolation, hyper-arousal reactions including anger outbursts. Operation Red Wings Foundation’s Post-traumatic Growth Programs include education for Service Members, Veterans and their family members on the warning signs, symptoms and characteristics of these injuries, and provide skills and resources for continued recovery.

These self-assessment questions are not intended
to provide a diagnosis or substitute for a professional evaluation. Self- assessment questions obtained from MyHealth.VA.Gov.
The following questions are a list of problems and complaints that Service Members, Veterans sometimes
have in response to stressful military experiences.

The following self-assessment questions are not intended
to provide a diagnosis or substitute for a professional evaluation. TBI symptoms obtained from the Mayo Clinic.
Traumatic brain injury can have wide-ranging physical and psychological effects. Some signs or symptoms may appear immediately after the traumatic event, while others may appear days or weeks later. The signs and symptoms of mild traumatic brain injury may include:
If you are experiencing many of the symptoms above, you may be experiencing symptoms of a Traumatic Brain Injury. For a formal diagnosis and evaluation, please consult your physician.
The following information is summarized from an article written by Lorie T. DeCarvalho, PhD for the National Center for PTSD.
According to the International Association for the Study of Pain (IASP), chronic pain involves suffering from pain in a particular area of the body (e.g., in the back or the neck) for at least three to six months. Chronic pain may be as severe as, if not more severe than, acute pain but the individual’s experience
is “modulated and compounded by the prolonged or recurrent nature of the chronic state, and further complicated by a multitude of economic and psychosocial factors”. In stark contrast to acute pain, chronic pain persists beyond the amount of time that is normal for an injury to heal. Chronic pain can have a variety of sources including disease
processes or injuries. Some chronic pain stems from a traumatic event, such as a physical or sexual assault, a motor vehicle accident, or some type of disaster. Under these circumstances, the person may experience both chronic pain and Post-traumatic Stress Disorder (PTSD).
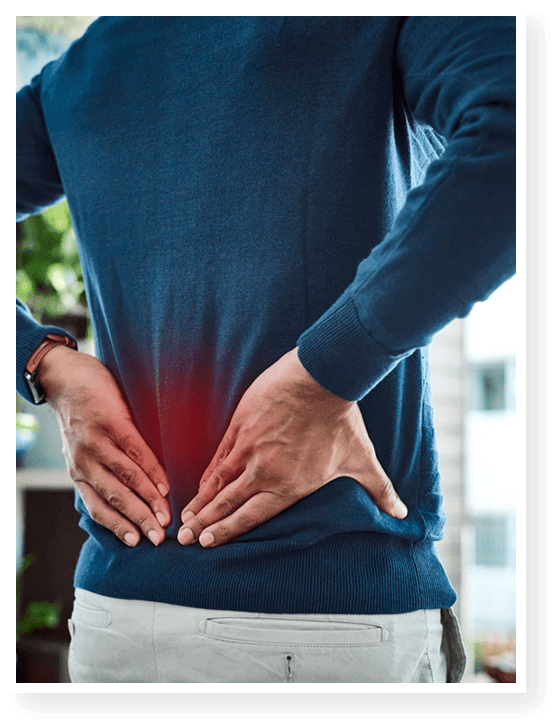
There are many forms of chronic pain, and each type of condition results in different experiences of pain and disability. As an example, chronic low back pain (CLBP), the most pervasive or common type of pain, is known to result in severe disability and limitation of movement.
Most patients with chronic pain resort to invasive assessment or treatment procedures, including surgery, to help relieve the pain. Individuals with chronic pain are less able to function in daily life than those who do not suffer from chronic pain. Patients with severe chronic pain and limited mobility oftentimes are unable to perform activities of daily living, such as walking, standing, sitting, lifting light objects, doing paperwork, standing in line at a grocery store, going shopping, or working. Many patients with chronic pain cannot work because of their pain or physical limitations.
Chronic pain and the disability that often comes with it can lead to a cognitive reevaluation and reintegration of one’s belief systems, values, emotions, and feelings of self-worth. Numerous studies have indicated that many patients who experience chronic pain (up to 100%) tend also to be clinically depressed. In fact, depression is the most common psychiatric diagnosis in patients with chronic pain. The experience of progressive, consistent chronic pain and disability also translates for many individuals into having thoughts of suicide as a means of ending their pain and frustration.
The prevalence of PTSD is substantially elevated in patients with chronic pain. A current PTSD prevalence of 35% was seen in a sample of chronic pain patients, compared to 3.5% in the general population. In a study of patients with chronic low back pain, 51% of the patients evidenced significant PTSD symptoms. In another study of patients who experienced chronic pain following a motor vehicle accident, researchers found that 50% of the patients developed PTSD.
One symptom of PTSD is that the person becomes emotionally or physically upset when reminded of the traumatic event. For people with chronic pain, the pain may actually serve as a reminder of the traumatic event, which will tend to exacerbate the PTSD.

The Operation Red Wings Foundation is a Federal 501(c)(3) Non-Profit EIN: 27-1850918 Website and Contents
© 2023 Operation Red Wings Foundation. All Rights Reserved.